Microsurgical Breast Reconstruction
 The goal of breast reconstruction is to restore the appearance of a breast after mastectomy. Although the function of the breast is lost when it is removed for breast cancer, the appearance, shape and texture can be reconstructed to closely approximate a natural breast. Recent microsurgical advances allow for improved and safer reconstruction than was available even ten years ago. DIEP flap, SIEA flap and TUG flap microsurgical breast reconstruction have significant advantages over implant, pedicled TRAM and free TRAM reconstruction. Foremost, they lessen the expense of surgery at the donor area by decreasing the surgical burden on the donor tissue site.
The goal of breast reconstruction is to restore the appearance of a breast after mastectomy. Although the function of the breast is lost when it is removed for breast cancer, the appearance, shape and texture can be reconstructed to closely approximate a natural breast. Recent microsurgical advances allow for improved and safer reconstruction than was available even ten years ago. DIEP flap, SIEA flap and TUG flap microsurgical breast reconstruction have significant advantages over implant, pedicled TRAM and free TRAM reconstruction. Foremost, they lessen the expense of surgery at the donor area by decreasing the surgical burden on the donor tissue site.
Microsurgical DIEP, SIEA and TUG flap reconstruction can improve the aesthetics of the reconstructed breast and reduce complications such as fat necrosis and flap loss. Although microvascular autologous reconstruction can be surgically more complex and requires an increased operating time, the long term results have solidly established it as a superb method of reconstruction. Unfortunately, not many surgeons perform microsurgical breast reconstruction, or if they do, they perform it infrequently. Patients may be discouraged from seeking out microsurgical reconstruction as a result.
Although not offered by many plastic surgeons, microsurgical reconstruction with these flaps can be an excellent choice. These procedures offer potential for:
- Permanent results
- Sparing of abdominal muscles
- The aesthetic perk of a tummy tuck or inner thigh lift
- Breasts that feel more soft and genuine than implants do
- Breasts that look more natural than implants do
Donor Tissue Area
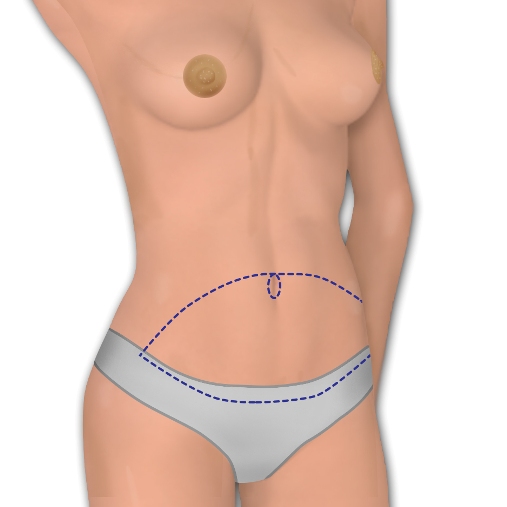
Tissue from the abdomen provides a large amount of skin and subcutaneous fat with an excellent blood supply. The most common technique for autologous reconstruction is the TRAM flap. The TRAM provides the advantages of abdominal tissue, but requires removal of part or all of the rectus muscles from the abdomen and some of the fascia of the abdominal wall. One of the main reasons women have been seeking out microsurgical breast reconstruction is because they worry about the loss of abdominal muscles with the TRAM flap. A very popular form of reconstruction, TRAM flaps have become widely available and have produced excellent aesthetic results in many women. The TRAM was a major advance in breast reconstruction when it became available. The abdominal skin and fat is soft, feels like a breast and has all the advantages of using your own tissue. The results are permanent, and there is no need to worry about implant capsule formation or the changes in appearance over time that are associated with implants and capsular contracture.
DIEP
![]() The DIEP flap provides the abdominal skin and subcutaneous tissue the TRAM flap does while sparing the rectus muscles and fascia. Patients have decreased post-operative pain, less post-surgical abdominal wall weakness and a decreased chance of abdominal wall hernia formation. The extent of fascial and muscle dissection is dependent on the anatomy and surgeon experience. Anatomical variations between patients are significant and can reveal medial, central or lateral perforator systems, each with variable courses through the muscle. Although most patients can have their flaps harvested on a single perforator, many may need a second if there is no large primary perforator.
The DIEP flap provides the abdominal skin and subcutaneous tissue the TRAM flap does while sparing the rectus muscles and fascia. Patients have decreased post-operative pain, less post-surgical abdominal wall weakness and a decreased chance of abdominal wall hernia formation. The extent of fascial and muscle dissection is dependent on the anatomy and surgeon experience. Anatomical variations between patients are significant and can reveal medial, central or lateral perforator systems, each with variable courses through the muscle. Although most patients can have their flaps harvested on a single perforator, many may need a second if there is no large primary perforator.
SIEA
![]() Like the DIEP, the SIEA flap provides the same abdominal skin and fat, but it relies on a different blood supply and requires less surgical dissection than the DIEP flap. The SIEA vessels can be quite small and present different anatomic challenges for insetting at the recipient area. The vessels lack the more flexible leash the DIEP vessels have. And, the size of the flap artery is almost always a mis-match with the internal mammary. In addition, patients that have had previous abdominal surgery (such as a c-section) may not have usable SIEA vessels as a result of the previous surgery. Hernia formation is exceedingly rare.
Like the DIEP, the SIEA flap provides the same abdominal skin and fat, but it relies on a different blood supply and requires less surgical dissection than the DIEP flap. The SIEA vessels can be quite small and present different anatomic challenges for insetting at the recipient area. The vessels lack the more flexible leash the DIEP vessels have. And, the size of the flap artery is almost always a mis-match with the internal mammary. In addition, patients that have had previous abdominal surgery (such as a c-section) may not have usable SIEA vessels as a result of the previous surgery. Hernia formation is exceedingly rare.
TUG
![]() The TUG flap flap relies on tissue from the inner upper thigh as well as a portion of the gracilis muscle. This tissue is similar to the skin and fat removed in the cosmetic medial thigh lift procedure. Loss of the gracilis muscle, unlike the rectus muscle, does not lead to hernia formation or loss of strength. Although the TUG flap usually has good sized blood vessels, they can on occasion be quite small. And the amount of tissue that is supplied by the inner thigh tends to be less than there is available in most patients on the abdomen.
The TUG flap flap relies on tissue from the inner upper thigh as well as a portion of the gracilis muscle. This tissue is similar to the skin and fat removed in the cosmetic medial thigh lift procedure. Loss of the gracilis muscle, unlike the rectus muscle, does not lead to hernia formation or loss of strength. Although the TUG flap usually has good sized blood vessels, they can on occasion be quite small. And the amount of tissue that is supplied by the inner thigh tends to be less than there is available in most patients on the abdomen.
The shape of the TUG flap provides superior projection when compared to abdominal tissue. And the inner thigh skin mimics a nipple areola complex unusually well, when shaped correctly.
TRAM
![]() But the TRAM flap has some significant drawbacks. It requires removal of part or most of a rectus muscle and part of the rectus fascia. The rectus muscle provides abdominal strength and support. In bilateral TRAM flaps (used to reconstruct both breasts or a large single breast), function in both rectus muscles is lost, and more fascia is sacrificed. In some TRAMS the abdominal wall may need synthetic reinforcement of the rectus fascia.
But the TRAM flap has some significant drawbacks. It requires removal of part or most of a rectus muscle and part of the rectus fascia. The rectus muscle provides abdominal strength and support. In bilateral TRAM flaps (used to reconstruct both breasts or a large single breast), function in both rectus muscles is lost, and more fascia is sacrificed. In some TRAMS the abdominal wall may need synthetic reinforcement of the rectus fascia.
The ability to perform a sit-up may be lost lost with TRAM flaps, resulting in patients needing to roll on their side before getting out of bed or lying down. The loss of abdominal support can also lead to hernia formation and bulging.
Procedure Selection
The unique history, circumstances and goals of each specific patient help to define the choice of a reconstruction method. No single technique is applicable to everyone. Some patients may be better candidates for implants, an expander or latissimus reconstruction. Or, for one reason or another, they choose to have implant reconstruction. Although technically more complex, the potential benefits of microsurgical reconstruction can be significant relative to implant or TRAM reconstruction.
Other concurrent factors, like chemotherapy and radiation, physical health, body habitus and patient goals, makes it impossible to cover all the aspects and decision making possibilities in these pages. All these factors play a role in the choice, timing and outcome of reconstruction.